DOP16 An evaluation of the exposure–efficacy relationship for subcutaneous vedolizumab maintenance treatment of Crohn’s disease: Pharmacokinetic findings from VISIBLE 2
C. Chen1, M. Rosario2, D. Polhamus3, N. Dirks3, W. Zhang4, W. Sun1, K. Kisfalvi5, B. Feagan6, W. Sandborn7, S. Vermeire8, G. D’Haens9
1Takeda, Quantitative Clinical Pharmacology, Cambridge, USA, 2Takeda, Clinical Pharmacology, Deerfield, USA, 3Metrum Research Group, Tariffville, USA, 4Takeda, Statistical and Quantitative Sciences, R&D, Cambridge, USA, 5Takeda, Research and Development, Global Clinical Sciences, Cambridge, USA, 6Western University, Robarts Clinical Trials, London, Ontario, Canada, 7Division of Gastroenterology, University of California San Diego, La Jolla, USA, 8Department of Gastroenterology, University Hospitals Leuven, Leuven, Belgium, 9Department of Gastroenterology, Amsterdam University Medical Centers, Amsterdam, The Netherlands
Background
The exposure–efficacy relationship and immunogenicity rates of the new vedolizumab subcutaneous (SC) formulation have been established for maintenance treatment of ulcerative colitis (UC).1 Here, we report vedolizumab SC exposure–efficacy and immunogenicity in Crohn’s disease (CD).
Methods
VISIBLE 2 (NCT02611817; EudraCT 2015-000481-58) was a pivotal, phase 3, randomised, double-blind, placebo-controlled trial evaluating the efficacy and safety of vedolizumab SC (108 mg every 2 weeks) as maintenance treatment in patients with moderately to severely active CD. Following intravenous (IV) vedolizumab (300 mg Week 0 and 2) induction, patients with a clinical response at Week 6 (≥70-point decrease in CD activity index [CDAI] from Week 0) were randomised to blinded maintenance treatment and included in the analyses. Vedolizumab serum concentrations were measured prior to dosing using an enzyme-linked immunosorbent assay. Immunogenicity was assessed with a drug-tolerant electrochemiluminescence assay. Predicted vedolizumab trough concentrations at Week 52 were grouped by quartiles (Q), and Week 52 efficacy outcome rates calculated for each Q. Missing efficacy outcome data were imputed as failures. Efficacy outcomes were clinical remission (CDAI ≤150) and enhanced clinical response (≥100-point decrease in CDAI from Week 0 at Week 52).
Results
Following vedolizumab IV induction (
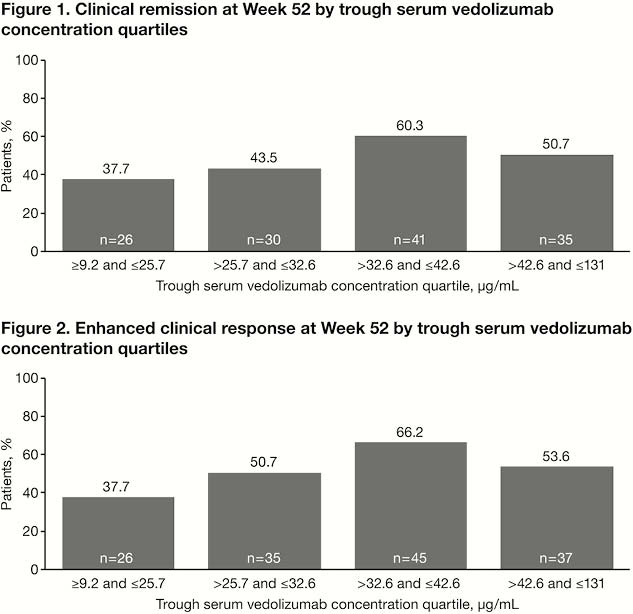
Conclusion
These preliminary results suggest a trend for higher vedolizumab SC serum concentrations with greater efficacy in CD, but the association was less pronounced than was reported in UC. (1) The AVA rate was similar to what was observed in prior vedolizumab IV studies. (2) In this study, vedolizumab immunogenicity appeared to be associated with clinical outcome.
Sandborn WJ,
Sandborn WJ,


