S. Lin1,2, N. Chanchlani1,2, B.M. Invergo3, M.W. Anderson3, H.M. Guay4, M. Reppell4, J.W. Butler4, J.R. Goodhand1,2, T. Ahmad1,2, N.A. Kennedy1,2, Exeter IBD Pharmacogenetics Research Group
1Exeter IBD Pharmacogenetics Research Group, University of Exeter, Exeter, UK, 2Department of Gastroenterology, Royal Devon and Exeter NHS Foundation Trust, Exeter, UK, 3Translational Exchange @ Exeter- Living Systems Institute, University of Exeter, Exeter, UK, 4Department of Research and Development, AbbVie Inc., North Chicago, USA
Background
Proteomic biomarkers have been linked to anti-TNF treatment failure, but previous studies have been insufficiently powered to stratify associations by drug level. The Personalised Anti-TNF Therapy in Crohn’s disease (PANTS) is a prospective UK-wide study investigating treatment failure in 1610 anti-TNF naïve patients. We aimed to identify proteomic markers of treatment failure.
Methods
We sampled patients with primary non-response (PNR) (n = 223) and remission (n = 219) who had a baseline CRP ≥4 mg/l and/or calprotectin >100 µg/g. PNR was defined at week 14 as ongoing steroids, or both of HBI failed to fall by ≥3 points or to ≤4 and CRP failed to fall by ≥50% or to ≤3 mg/l. Non-remission at week 54 was defined as HBI >4 and CRP >3 mg/l and no steroids. Targeted serum proteomic analysis of 180 proteins using Olink Inflammation and Immune Response panels were performed. Mann–Whitney U tests were used to identify baseline proteins that predicted PNR and non-remission. Sub-group analyses stratified by drug level were undertaken. Pharmacokinetic (PK) failure was defined as PNR with low drug level (infliximab level <2 mg/l, adalimumab level <6 mg/l) and pharmacodynamic (PD) failure as PNR despite adequate drug level. Significant proteins were entered into multivariable logistic regression models and Bayesian information criterion (BIC) with backward stepwise selection were used to build predictive models of treatment failure. We applied 10-fold cross-validation to test the models. P-values of < 0.05 were considered significant.
Results
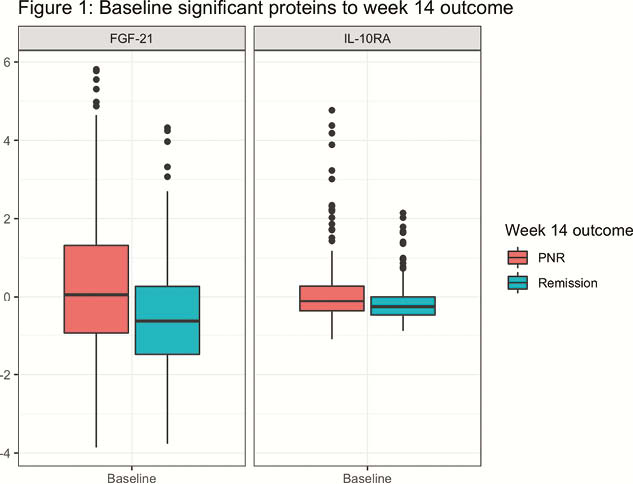
Elevated fibroblast growth factor 21 (FGF21) (OR 1.3, CI 1.1–1.4, p = 3.4 × 10–5) and interleukin-10 receptor subunit α (IL10RA) (OR 1.6, CI 1.2–2.1, p = 6.3 × 10–4) predicted PNR (Figure 1). At week 14, FGF21 (OR 1.5, CI 1.3–1.9, p = 1.8 × 10–6) and IL10RA (OR 1.8, CI 1.3–2.3, p = 5.8 × 10–5) levels were also associated with PNR.
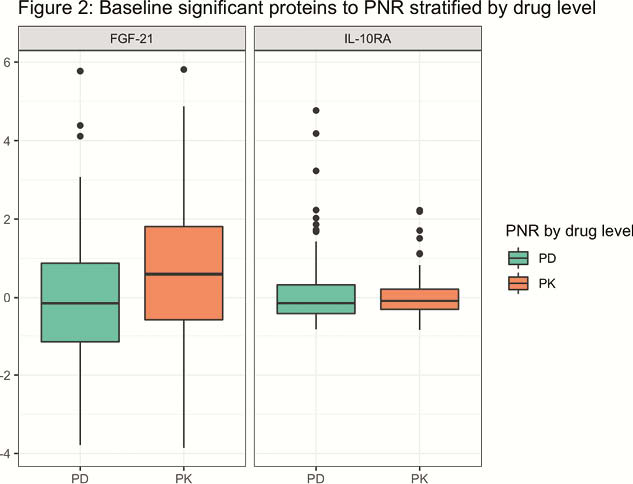
Sub-group analyses showed baseline FGF21 (OR 1.4, CI 1.2–1.7, p = 2.0 × 10–4) predicted PK failure and that IL10-RA (OR 1.6, CI 1.1–2.2, p = 6.7 × 10–3) predicted PD failure (Figure 2).
In separate models, non-remission at week 54 was predicted by baseline (FGF21; OR 1.3, CI 1.1–1.4, p = 1.4 × 10–4, IL10-RA; OR 1.5, CI 1.1–2.0, p = 3.6 × 10–3) and week 14 (FGF21; OR 1.4, CI 1.2–1.7, p = 3.6 × 10–4, IL10-RA; OR 1.7, CI 1.3–2.4, p = 1.7 × 10–4) FGF21 and IL10-RA levels. Model validation of baseline FGF21 and IL10-RA showed an area under the curve of 0.61 (CI 0.57–0.64) for PNR and 0.60 (CI 0.56–0.64) for non-remission at week 54.
Conclusion
Our study identified FGF-21 and IL10-RA as proteins of interest associated with PK and PD treatment failure, respectively. Functional studies to determine the molecular mechanism driving dysregulation of these proteins are required.




