P005 Regulators of the guanylate cyclase pathway are potential novel markers of mucosal healing in IBD
L.E. Jeffery1, U.N. Shivaji1, D. Zardo2, A. Acharjee3, O.M. Nardone4, S.C. Smith4, G. Gkoutos3, S.S. Visweswariah5, S. Ghosh1, M. Iacucci1
1NIHR Birmingham Biomedical Research Centre, University of Birmingham, Gastroenterology, Birmingham, UK, 2University Hospitals Birmingham, Pathology, Birmingham, UK, 3Department of Gastroenterology, Institute of Cancer and Genomic Sciences, University of Birmingham, Birmingham, UK, 4Department of Gastroenterology, Institute of Immunology and Immunotherapy, University of Birmingham, Birmingham, UK, 5Department of Molecular Reproduction, Development and Genetics, Indian Institute of Science, Bangalore, India
Background
Intestinal guanylate cyclase C (GC-C) present in epithelial cells has been shown to have a role in gut homeostasis. The downstream effects of activation of GC-C are due to production of cyclic-GMP. GC-C is encoded by the gene
Methods
Forty-four patients with IBD and 7 patients with polyps (controls) at University Hospitals Birmingham, UK were recruited under ethical consent. Relevant demographic and clinical data were extracted from the hospital EMR. All patients had disease activity recorded on endoscopic examination of mucosa and intestinal biopsies collected for analysis. Mucosal healing was defined as MES = 0 (UC) and SES-CD <6 (CD). Of 44 patients, 14 had matched baseline and 12-week post-biologic therapy assessment and had tissues collected. Intestinal biopsies were analysed by 3’RNA-sequencing using the Illumina Nextseq sequencer. FASTQ files were generated through BaseSpace and reads de-multiplexed, trimmed, aligned, and quantified using the GeneGlobe (Qiagen) workflow. Expression was compared between groups using either Wilcoxon tests or Kruskal–Wallis with Dunn post-hoc analysis as appropriate.
Results
Expression of Guanylate cyclase activators
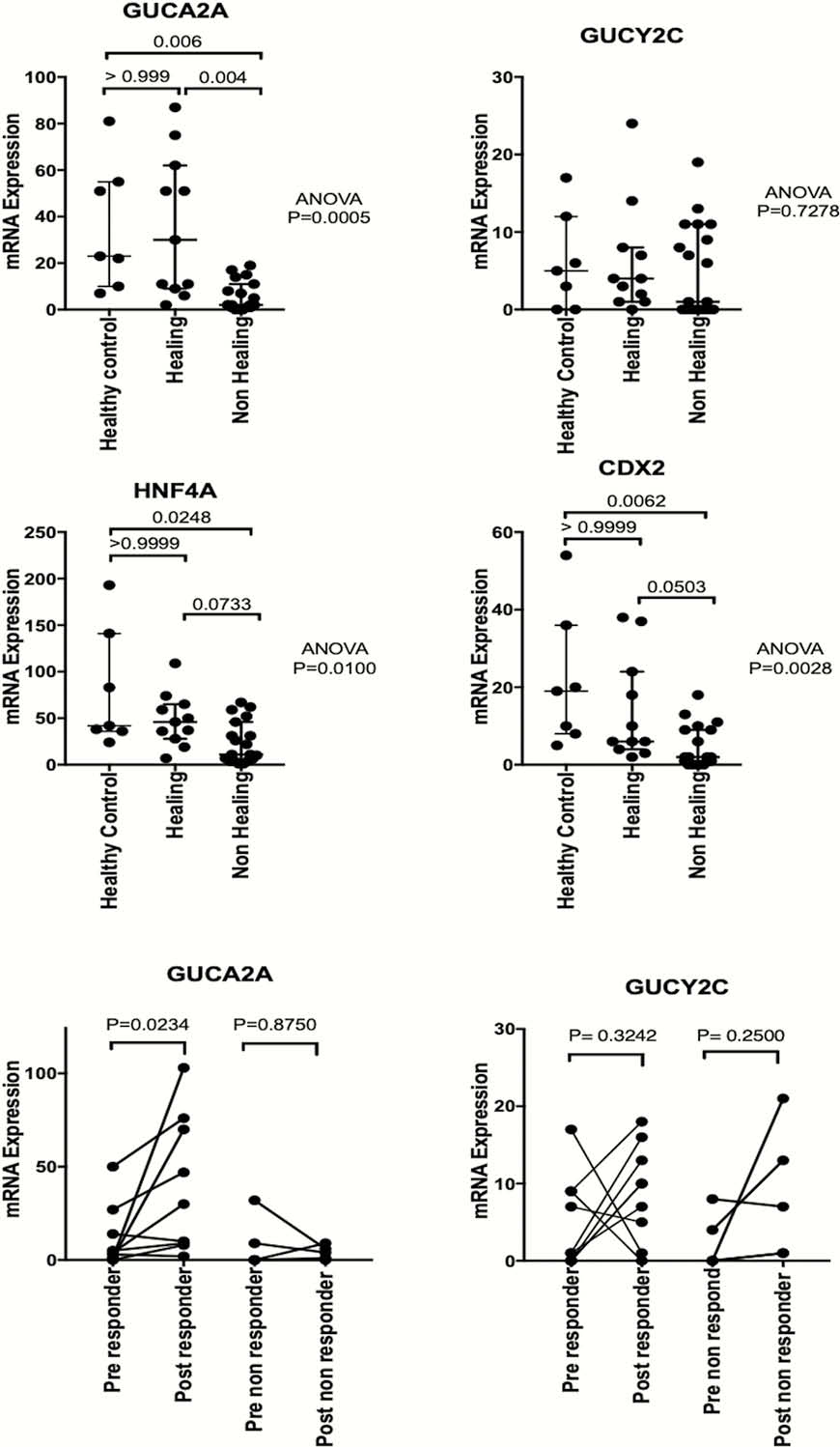
Conclusion
Our findings suggest that regulation of the Guanylate Cyclase pathway may be involved in the restoration of a stable mucosa in IBD and that expression of its regulators may be used to indicate response to treatment.


