P022 Impact of increasing disease symptom concordance between patients with inflammatory bowel disease and their physicians: insights from US, France, Germany, Italy, Spain and UK (5EU)
J. Kershaw1, R. Wild1, R. Lukanova1, S. Bruce Wirta2, M. Sikirica3
1Adelphi Real World, Adelphi, Manchester, UK, 2Janssen-Cilag, Janssen, Solna, Sweden, 3Janssen Scientific Affairs, LLC, Janssen, Horsham- PA, USA
Background
Accurate disease activity assessment builds on dialogue between patients with CD and UC and their doctors and is key for management of IBD.
Methods
Assess the level of patient and physician symptom concordance on disease, health-related quality of life (HrQol), work productivity and patient satisfaction using the Adelphi Disease-Specific Programme.
Results
Cross-sectional study among CD and UC patients and their gastroenterologists in US and 5EU. Data were collected in two waves, from November 2014–March 2015, and September 2017–January 2018, and then merged. Physicians completed patient record forms (PRFs) for the next seven UC and eight CD patients; same patients completed patient self-completion (PSC) forms describing how UC/CD affected them. PRFs collected diagnosis data, disease history, symptoms, treatment and management history. PSCs collected similar data, including patient reported outcome measures to assess the humanistic burden. Patients were grouped based on degree of alignment with physicians in symptom reporting (full agreement, discordance on 1–4 symptoms, discordance on 5+ symptoms out of 22 symptoms). Comparisons between groups were made using Chi-squared and Kruskal–Wallis for continuous and categorical variables.
Conclusion
A total of 2524 CD and 2153 UC patients were included in the analysis (mean age CD 38.5/UC 40.3, CD 50.2% male/UC 52.0%, mean time since diagnosis CD 5.6 years/UC 5.1 years). There was overall reasonable agreement in symptom reporting between patients and their physicians; however, amongst 17% of UC and CD patients and physicians, there was discordance on 5+ symptoms. Higher symptom concordance significantly associated with better patient outcomes: higher remission rates, productivity, HrQoL scores and satisfaction (Table 1).
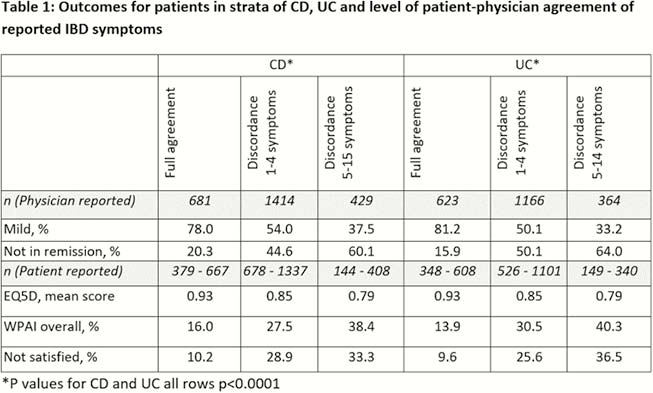
We observed moderate discordance between patient and physician reporting of current UC and CD symptoms. While even small discordance was associated with worse clinical outcomes: HrQol, productivity and satisfaction. Future studies are needed to improve understanding of the reasons behind discordance and association with worsened outcomes.


