P133 Pregnancy in inflammatory bowel disease: experience of a Chilean cohort
P. Núñez1, E. Sepúlveda2, D. Simian3, C. Figueroa3, L. Flores3, P. Ibáñez3, U. Kronberg4, J. Lubascher3, G. Pizarro3, R. Quera3
1San Juan de Dios Hospital, Gastroenterology Department – IBD Fellow Clínica Las Condes, Santiago, Chile, 2Clínica Las Condes, Gynecology and Obstetrics Department, Santiago, Chile, 3Clínica Las Condes, Gastroenterology Department – Inflammatory Bowel Disease Program, Santiago, Chile, 4Clínica Las Condes, Surgery Department, Colorectal Unit – Inflammatory Bowel Disease Program, Santiago, Chile
Background
In inflammatory bowel disease (IBD), a high percentage of women are diagnosed during their reproductive age. IBD in remission is the ideal scenario when planning a pregnancy. Here, we describe the demographic, clinical and pregnancy/childbirth characteristics in patients with IBD treated at a tertiary centre in Chile between 2017 and 2019.
Methods
Observational, analytic study. We retrospectively reviewed women diagnosed with IBD who were pregnant or delivered during the study period. Demographic, clinical, obstetric and delivery data were obtained from the IBD registry, approved by the local IRB. Descriptive statistics and association tests performed (
Results
Forty-six women with IBD were included (Tables 1). At the beginning of pregnancy, 19 (41%) had active disease and 27 (59%) were in remission. Of those with active disease, 8 (79%) remained active and six had spontaneous abortions. In those who were in remission, 20 (74%) remained in this condition. Six patients (13%) discontinued treatment (four based on external medical advice, two on her own). Preconception counselling was performed in 16/40, group with a higher percentage of remission during pregnancy (69% vs. 25%,
| Age (median; range) | 32 (24–41) |
| Ulcerative colitis | 33 (72) |
| Crohn’s disease | 12 (26) |
| Non-classifiable IBD | 1 (2) |
| Years of disease (median; range) | 6 (1–19) |
| Ulcerative colitis (extent) | |
| Pancolitis | 18 (55) |
| Left colon | 9 (27) |
| Proctitis | 6 (18) |
| Crohn’s disease (localisation) | |
| L1: terminal ileon | 4 (33) |
| L2: colon | 3 (25) |
| L3: Ileocolonic | 5 (42) |
| L4: upper gastrointestinal | 0 (0) |
| Crohn’s disease (behaviour) | |
| B1: non stricturing non penetrating | 10 (83) |
| B2: Stricturing | 2 (17) |
| B3: penetrating | 0 (0) |
| Perianal disease | 2 |
| Biological agents | 9 (19) |
| Adalimumab | 3 |
| Infliximab | 6 |
| Thiopurines | 15 (33) |
| Aminosalicylates | 22 (48) |
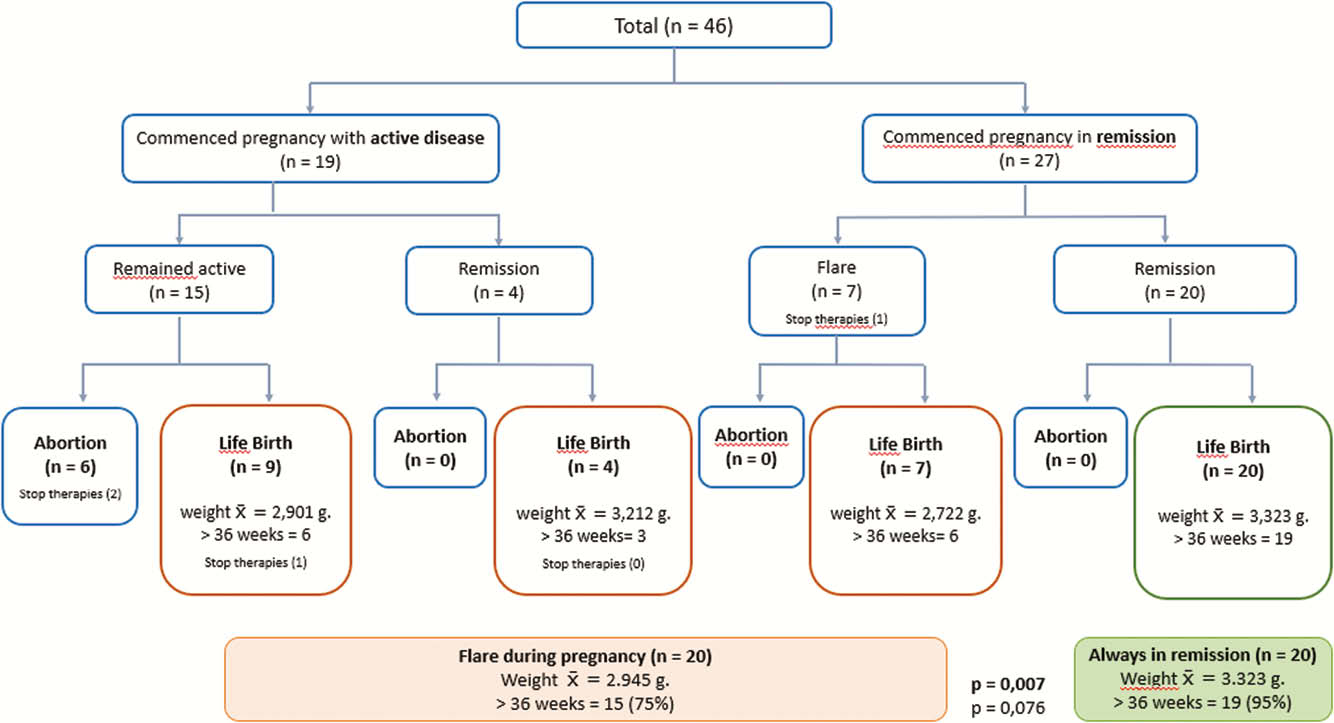
Conclusion
In this cohort, we observed that pregnancy during remission presents better outcomes and that preconception counselling would allow a better IBD control during pregnancy.


