P183 The prevalence of incidental terminal ileitis in persons undergoing non-diagnostic colonoscopy: a meta-analysis
M. Agrawal1, M. Bento-Miranda2, S. Walsh3, J.F. Colombel1, R. Ungaro1
1Icahn School of Medicine at Mount Sinai- New York, The Dr Henry D. Janowitz Division of Gastroenterology, New York, USA, 2Hospital and University Center of Coimbra – Portugal, Division of Gastroenterology, Coimbra, Portugal, 3Icahn School of Medicine at Mount Sinai – New York, Levy Library, New York, USA
Background
Incidentally diagnosed terminal ileitis has been reported among asymptomatic persons undergoing non-diagnostic colonoscopy. The purpose of our study was to determine the prevalence and long-term outcomes of asymptomatic terminal ileitis.
Methods
We developed and executed a systematic search strategy in three biomedical databases (Medline, Embase and Web of Science) and relevant scientific meeting abstracts, from inception to May 1, 2019, to identify observational studies that reported the prevalence of asymptomatic terminal ileitis in adults undergoing screening or polyp surveillance colonoscopy, and/or the long-term outcomes of such lesions. A random-effects meta-analysis was conducted to determine the pooled prevalence rate, confidence interval (CI), and report the heterogeneity score
Results
Of 2388 eligible studies, 1784 were screened after excluding duplicates, 84 were reviewed in full text and 14 studies were eligible for inclusion. Eight studies reported the prevalence of asymptomatic terminal ileitis in 46,460 persons undergoing non-diagnostic colonoscopy, and eight (two of eight reporting prevalence) studies reported follow-up data. The pooled rate of asymptomatic terminal ileitis was 1.5% (CI 1.0%, 16.3%), with
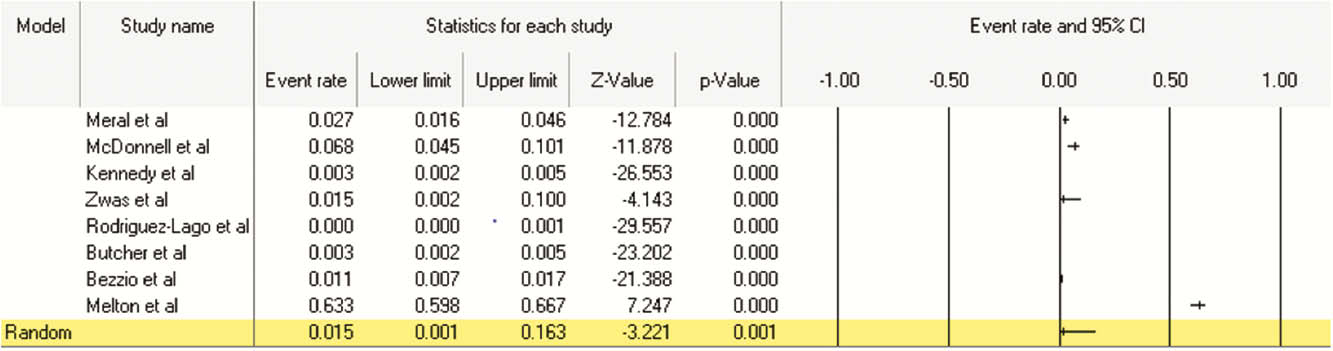
Conclusion
Asymptomatic terminal ileitis can be found incidentally in 1.5% of non-diagnostic colonoscopies. Based on limited data, the rate of its progression to overt CD seems low, and watchful waiting could likely be a reasonable strategy. More long-term follow-up studies are needed to inform the natural history of incidental terminal ileitis, factors that predict progression to CD and therapeutic implications.


