P219 Disease-specific avoidance is a predictor for fatigue in inflammatory bowel disease patients
L. Fierens1, I. Van de Pavert2, M. Walentynowicz2, S. Coenen1,3, P. Geens3, E. Weyts3, L. Van Oudenhove1,4, J. Vlaeyen2, A. von Leupoldt2, G. Van Assche1,3, S. Vermeire1,3, M. Ferrante1,3, I. Van Diest2
1Translational Research Center for Gastrointestinal Disorders TARGID- Department of Chronic Diseases, Metabolism, and Ageing, KU Leuven, Leuven, Belgium, 2Health Psychology Research Group, KU Leuven, Leuven, Belgium, 3Department of Gastroenterology and Hepatology, University Hospitals Leuven, KU Leuven, Leuven, Belgium, 4Dartmouth College, Cognitive and Affective Neuroscience Lab- Hanover- NH, USA
Background
A substantial group of patients with inflammatory bowel disease (IBD) experience fatigue, even while in clinical remission. At present, disease-specific behaviours that maintain or worsen symptom burden including fatigue have not been explored. We developed a questionnaire evaluating IBD-specific avoidance behaviour and investigated how this relates to self-reported fatigue.
Methods
This study was a close collaboration between the psychology and gastroenterology department of our tertiary referral centre. A 72-item IBD-specific avoidance behaviour questionnaire (IBD-B) was generated based on literature review and input from clinicians and a patient focus group (
Results
At wave 1, 46% and 69% of CD and UC patients, respectively, were in clinical remission. PCA suggested a reduction of the 72-item to a final 25-item IBD-B and a seven-factor solution for use in clinical practice (loading factors >0.5, Table 1). The final 25-item IBD-B showed good psychometric properties. The median (IQR) total IBD-B and fatigue scores were, respectively, 29 (40-20) and 52 (77-25) for patients in clinical remission compared with 38 (48-28) and 74 (87-50) for patients not in clinical remission (both

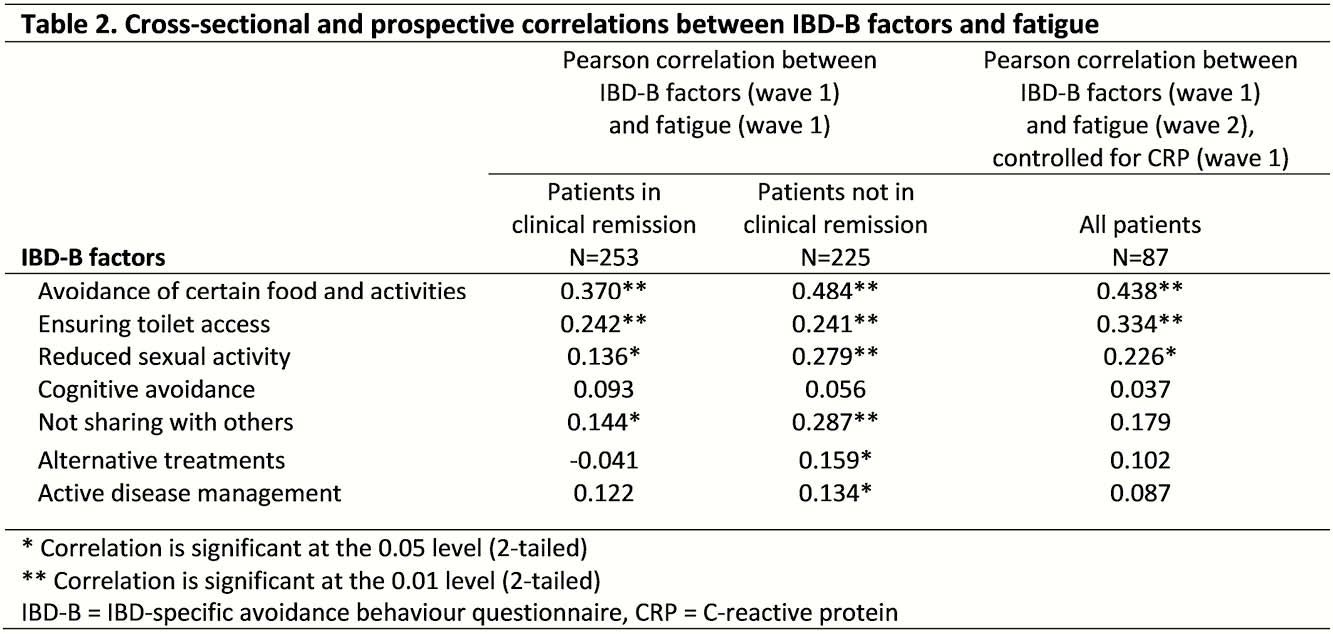
Conclusion
The IBD-B is a valuable tool to accurately measure IBD-specific avoidance behaviour in IBD patients. IBD patients without clinical remission report higher IBD-B values and show a higher correlation between avoidance behaviour and fatigue. Further research should now focus on identifying predictors for fatigue in IBD patients in clinical remission.


