P250 Root cause analysis to identify missed opportunities for the diagnosis of colorectal cancer in inflammatory bowel disease
C. Gordon1, D. Chee1, B. Hamilton1, N. Chanchlani1, N.M. Heerasing1, P. Hendy1, S. Lin1, E. Wesley1, I. Daniels2, J.R. Goodhand1, N.A. Kennedy1, T. Ahmad1
1Royal Devon and Exeter NHS Foundation Trust, Gastroenterology, Exeter, UK, 2Royal Devon and Exeter NHS Foundation Trust, Colorectal Surgery, Exeter, UK
Background
Colonoscopic surveillance in inflammatory bowel disease (IBD) patients leads to earlier detection of colorectal cancer (CRC) and reduces CRC-associated deaths. However, adherence to international surveillance guidelines in practice is poor. Consequently, we hypothesised that patients with IBD-associated CRC had suboptimal endoscopic surveillance and conducted a root cause analysis of IBD-associated CRC diagnoses to identify the scale of missed surveillance opportunities.
Methods
We calculated the incidence of CRC in our IBD population between 1998 and 2019 by cross-referencing the hospital’s CRC and IBD databases. All cases were adjudicated by IBD specialists to determine eligibility for surveillance using guidelines contemporaneous to the time of CRC diagnosis. For all eligible patients, a root cause analysis was conducted to determine whether there were missed opportunities to detect CRC.
Results
Our search identified 94 patients with IBD and CRC. We excluded 16 patients diagnosed with IBD after the diagnosis of CRC. The overall incidence of IBD-associated CRC in East Devon from 1998 to 2019 was 0.17% per year (95% CI 0.14 %–0.18%) with no statistically significant change seen over time (
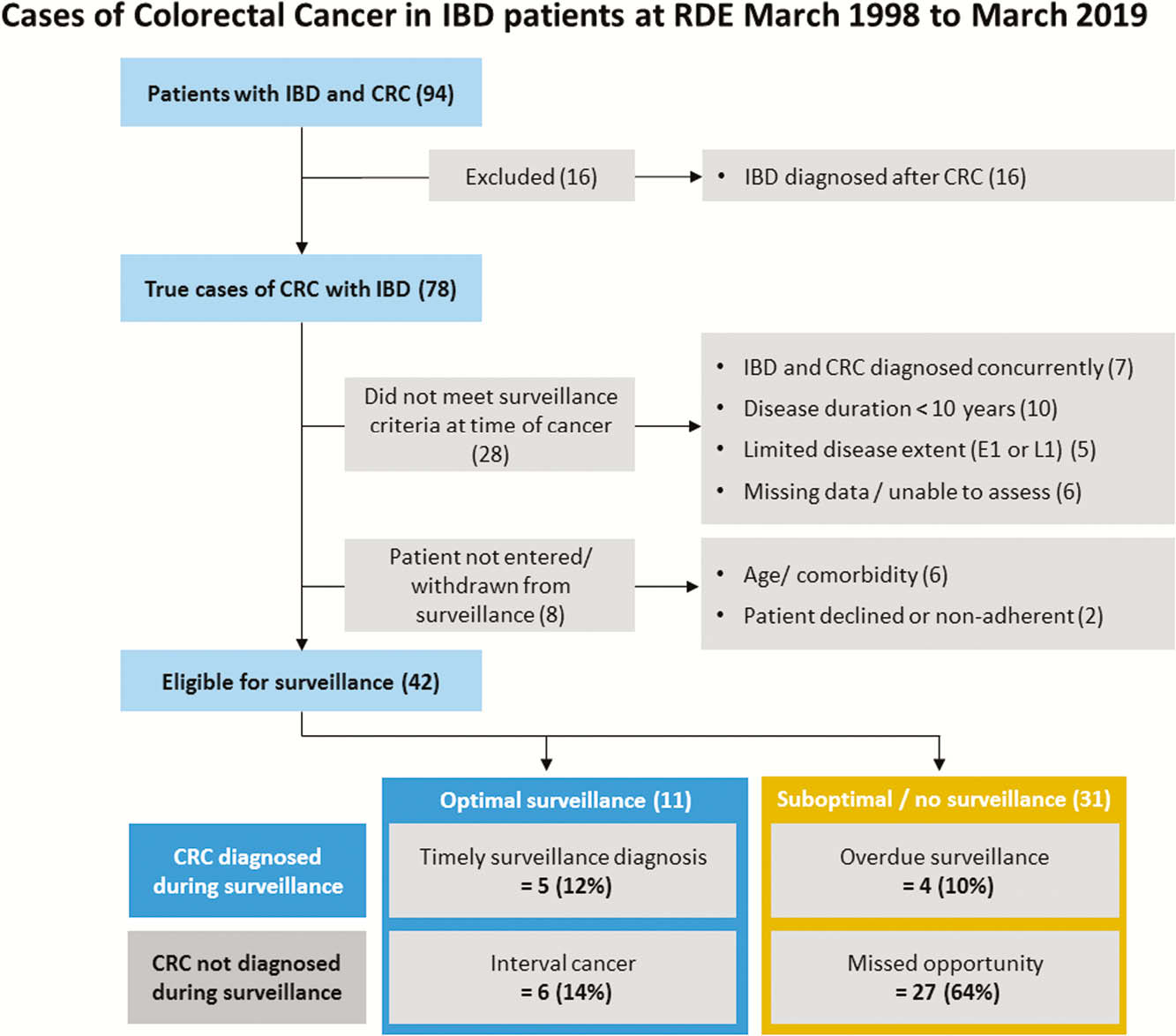
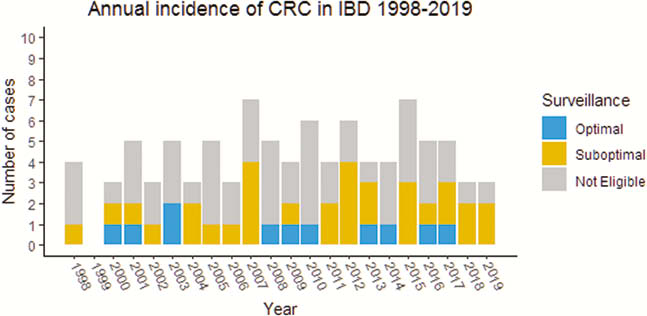
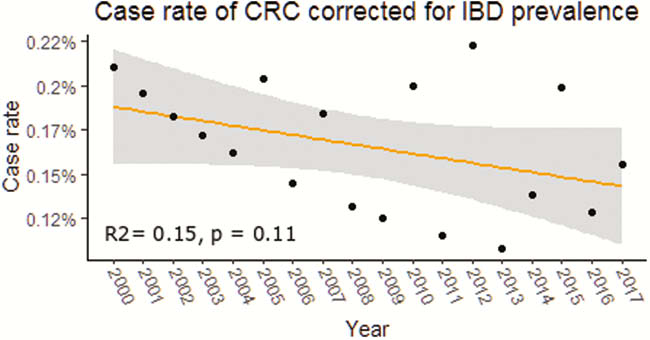
Conclusion
Two-thirds of patients who were eligible for surveillance had a missed opportunity to diagnose CRC. In most cases, the patient was known to the secondary care IBD service but no recommendation for surveillance was made. There is a need to implement processes to facilitate identification and recall of patients eligible for surveillance across primary and secondary care.


