P271 Trends in faecal calprotectin levels during pregnancy and post-partum in healthy women
J. Doherty1, R. Moore2, C. Kivlehan1, P. Twomey1, F. McAuliffe2, G. Cullen1
1Centre for Colorectal Disease, St Vincent’s University Hospital and School of Medicine- University College Dublin, Dublin, Ireland, 2UCD Obstetrics and Gynaecology Department, School of Medicine, University College Dublin, National Maternity Hospital, Dublin, Ireland
Background
Faecal calprotectin (FCP) is one of the most widely used non-invasive tools for diagnosis and assessment of inflammatory bowel disease (IBD). Numerous factors can influence FCP levels including weight, smoking status and medications. In clinical practise FCP is commonly used to identify flares during pregnancy. For a test that is widely used minimal data exists on the determinants of normal levels and variations in concentrations during pregnancy in healthy individuals. Our aim is to determine normal FCP levels during pregnancy and post-partum and whether levels change during pregnancy and post-partum in healthy individuals.
Methods
We performed a prospective study analysing FCP levels from pregnant women at 16- and 34-weeks’ gestation and 4- and 12-weeks post-partum. Basic demographics were collected including age, parity, medical history, BMI and smoking status. Patients with a history of gastrointestinal disorders were excluded. FCP concentrations were measured with a quantitative ELISA assay.
Results
98 patients were included in our study. 172 stool samples were collected for analysis. Sixty-two stool samples were collected at 16 weeks gestation, 48 samples from 34 weeks gestation, 38 samples from 4weeks post-partum and 24 samples from 12 weeks post-partum. The median age was 33 years (21–44). Forty-one patients had a BMI > 25 (42%). Sixteen patients were ex-smokers (16%) and one patient was actively smoking (1%). The median FCP levels from 16 weeks gestation was 29.5 (10–476), median level from 34 weeks gestation was 25.6 (10–259), from 4 weeks post-partum was 23.4 (10–318) and 12 weeks post-partum was 29.4 (10–216) (Table 1). There was no significant change in median FCP levels over the course of pregnancy and post-partum (p = 0.294). Interestingly median FCP levels were normal at all time points however we saw a slight numerical increase in FCP levels during pregnancy in patients whose BMI was > 25 and this reached statistical significance at 4weeks post-partum (p = 0.01) (Table 1, Graph 1). There was also a significant increase in FCP at 4 weeks post-partum in patients who were ex-smokers (
| Median FCP levels | 16weeks gestation | 34 weeks gestation | 4 weeks post-partum | 12 weeks post-partum |
| All patients | 29.5 | 25.6 | 23.4 | 29.4 |
| BMI > 25 | 66.4 | 53.6 | 78.5 | 48.3 |
| Ex-smokers | 48.7 | 30.5 | 62.8 | 38.1 |
| Multiparity | 68 | 53.3 | 26.1 | 53.7 |
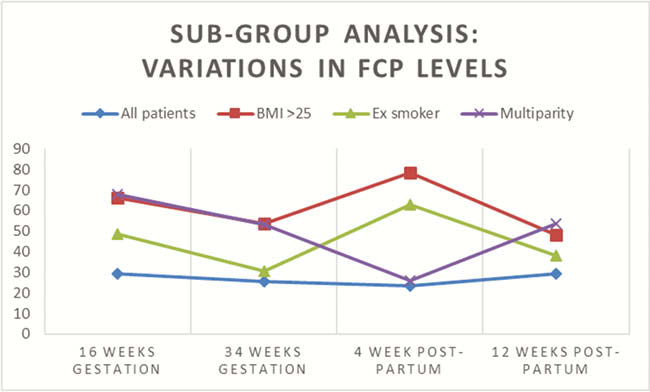
Conclusion
FCP levels are not affected by physiological changes in pregnancy or post-partum in normal healthy individuals without IBD. This confirms FCP is an effective tool for identifying flares of colitis during pregnancy. However, when using this tool, one should be aware that levels can be slightly altered by a patients’ smoking history and their weight and a detailed clinical history is essential when interpreting results.


