P303 Role of parietal healing by ultrasound in the evolution of patients with Crohn’s disease
P. Mayor Delgado, C.J. Suarez Ferrer, J. Poza Cordon, E. Martin Arranz, J.L. Rueda Garcia, M. Sanchez Azofra, M. Cuadros Martinez, M.A. Ruiz Ramirez, M.D. Martin Arranz
Hospital Universitario La Paz, Gastroenterology, Madrid, Spain
Background
The objective of this study is to assess the degree of parietal involvement with ultrasound and see how they influence the prognosis according to the findings.
Methods
It was defined as ‘parietal healing’ the normalisation of ultrasound findings in a previously affected segment (parietal thickness less than 3 mm and absence of parietal hyperaemia). Therefore, patients with absence of ultrasound activity but without reaching parietal healing were considered to be those without significant inflammatory signs (parietal thickness <4.5 mm and absence of hyperaemia or other inflammatory data) but who had not ‘normalised’ the previously affected segment.
Results
A total of 111 patients without ultrasound inflammatory activity were included. It was studied whether normalisation of parameters in a previously affected segment, i.e. parietal healing gave a better prognosis during follow-up. It was detected that 74 patients achieved ‘parietal healing’ and this subgroup of patients generally had a flare in 12% of cases (9/74 patients) compared with 27% of cases (10/37) among patients without parietal healing, these differences were statistically significant (
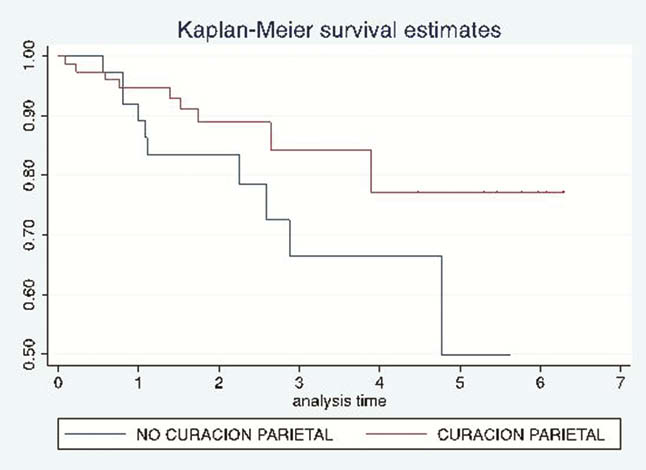
Conclusion
To conclude, detecting parietal healing by ultrasound improves prognosis by decreasing the number of outbreaks and increasing the median survival until outbreaks occur.


