P460 Evaluation of potential mechanisms underlying the safety observations of filgotinib in clinical studies in rheumatoid arthritis
A. Clarke, J. Di Paolo, B. Downie, A. Meng, N. Mollova, Y. Yu, P. Han
Clinical Development, Gilead Sciences Inc., Foster City- CA, USA
Background
Inhibitors of the Janus kinase-signal transducers and activators of transcription (JAK-STAT) pathway have demonstrated efficacy in the treatment of rheumatoid arthritis (RA) and inflammatory bowel disease (IBD). Differences in selectivity of JAK inhibitors for JAK1, JAK2, JAK3 and TYK2 may influence their respective safety profiles, and the mechanisms responsible are not currently known. Filgotinib (FIL), a JAK1 inhibitor, did not negatively impact haemoglobin, LDL:HDL ratios or natural killer (NK) cell counts in clinical trials. Here, we compare the
Methods
JAK inhibitors (FIL, FIL metabolite [GS-829845], baricitinib [BARI], tofacitinib [TOFA], and upadacitinib [UPA]) were evaluated
Results
Inhibition of cellular activity was calculated for each JAK inhibitor based on
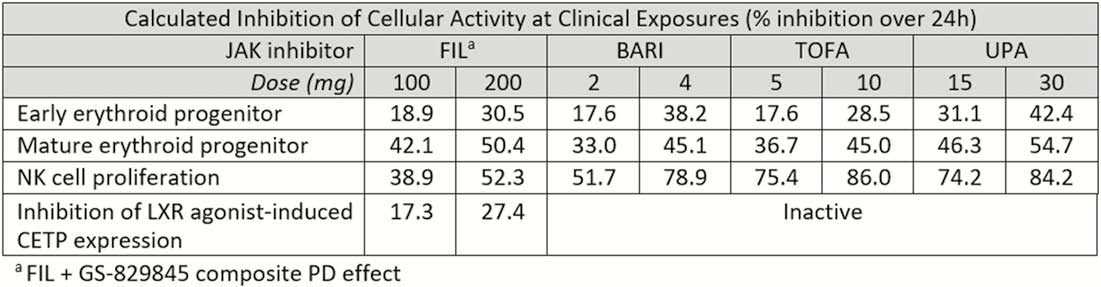
Conclusion
FIL, a JAK1 inhibitor, resulted in less inhibition of NK cell proliferation compared with BARI, TOFA, and UPA. FIL also reduced LXR agonist-induced CETP expression, while the other inhibitors did not alter these levels. These results provide a potential mechanistic link between the observed reduction of CETP concentration following FIL treatment and the previously observed reduction in the LDL:HDL ratio in RA patients.


