P507 United States and European patient perspectives on the impact of moderate-to-severe Ulcerative Colitis on sexual activity: Communicating Needs and Features of IBD Experiences (CONFIDE) survey
Travis, S.(1)*;Bleakman, A.(2);Dubinsky, M.(3);Rubin, D.(4);Panaccione, R.(5);Hibi, T.(6);Kayhan, C.(2);Gibble, T.H.(2);Sapin, C.(2);Flynn, E.(2);Atkinson, C.(7);Schreiber, S.(8);
(1)University of Oxford, Translational Gastroenterology Unit- John Radcliffe Hospital, Oxford, United Kingdom;(2)Eli Lilly and Company, Immunology, Indianapolis, United States;(3)Icahn School of Medicine, Pediatric Gastroenterology, New York, United States;(4)University of Chicago Medicine, Inflammatory Bowel Disease Center, Chicago, United States;(5)University of Calgary, Inflammatory Bowel Disease Group, Alberta, Canada;(6)Kitasato University, Center for Advanced IBD Research and Treatment, Tokyo, Japan;(7)Adelphi Real World, Research, Cheshire- England, United Kingdom;(8)University Hospital Schleswig-Holstein- Kiel University, Clinic for Internal Medicine 1, Kiel, Germany;
Background
Patients with ulcerative colitis (UC) report that UC negatively affects their quality of life (QoL), including sexual functioning, satisfaction, and drive.1,2 These effects are rarely discussed with or by gastroenterologists in clinical practice. The CONFIDE study aims to elucidate the impact of symptoms on the lives of patients with moderate-to-severe UC in the United States (US), Europe (EU5; France, Germany, Italy, Spain, and UK), and Japan. Data presented here are from the US and EU5.
Methods
Online, quantitative, cross-sectional surveys were conducted (July–September 2021). Criteria based on previous treatment, steroid use, and/or hospitalization were used to define moderate-to-severe UC. Data collected included patient perspectives on the impact of UC on sexual activity. Sexual activity was not limited to intercourse and included activities such as masturbation.
Results
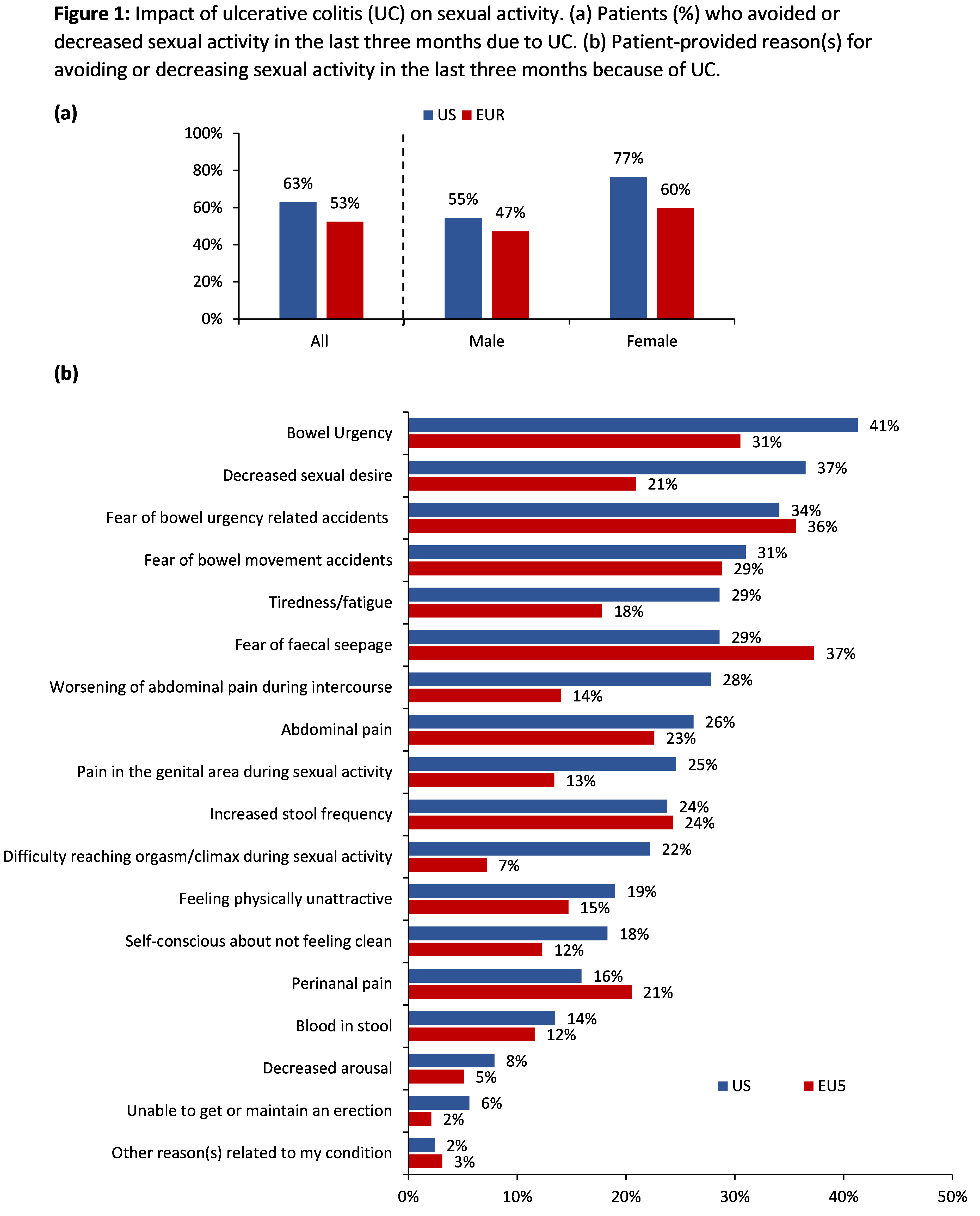
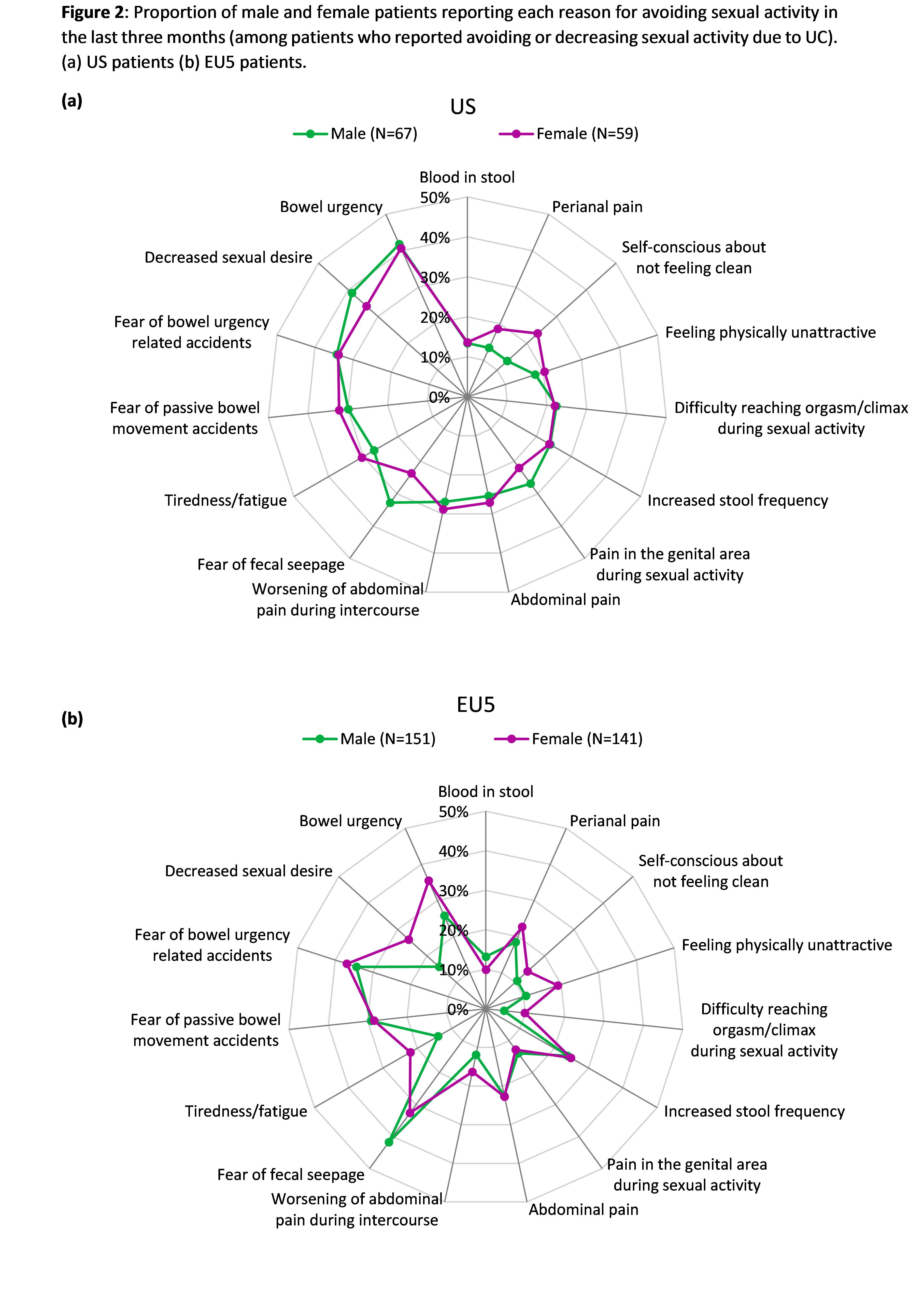
Surveys were completed by 200 US patients (male [M]=62%, mean age 40 years) and 556 EU5 patients (M=57%, mean age 39 years). Of these, 77% US and 54% EU5 patients were receiving advanced therapy (biologic/novel oral) and 52% and 73% were receiving steroids at the time of survey completion, respectively. Overall, 63% US patients (M=55%, female [F]=77%) and 53% EU5 patients (M=47%, F=60%) reported avoiding or decreasing sexual activity due to UC in the 3 months prior to the survey (Figure 1a). Among these patients (US: N=126; EU5: N=292), most frequently reported reasons for avoidance of sexual activity were bowel urgency (BU; 41%), decreased sexual desire (37%), and fear of BU-related accidents (34%) in the US and fear of faecal seepage (37%), fear of BU-related accidents (36%), and BU itself (31%) in EU5 (Figure 1b). Although reasons for avoiding sexual activity were broadly similar between sexes, higher percentage of male patients from both US and EU5 (US: M=33%, F=24%; EU5: M=42%, F=33%) reported fear of faecal seepage as a factor affecting sexual activity. Conversely, higher percentages of female patients reported perianal pain (M=13%, F=19%) and self-consciousness (M=13%, F=24%) as reasons for avoiding sexual activity in the US and decreased sexual desire (M=16%, F=26%), BU (M=26%, F=36%) and fatigue (M=14%, F=22%) in EU5 (Figure 2).
Conclusion
In both US and EU5 populations, >50% patients with moderate-to-severe UC reported avoiding or decreasing sexual activity due to UC, with bowel urgency and bowel urgency-related accidents being among the top three reasons. In addition to other QoL parameters, impact of UC on patients’ sexual health needs to be assessed in routine clinical practice.
References
1Bulut AE, et al. Turk J Gastroenterol. 2019;30:33-39.
2Jedel S, et al. Inflamm Bowel Dis. 2015;21:923-38.