P591 Negative impact of high body mass index on the efficacy of anti-TNFα agents in patients with Inflammatory Bowel Disease
Hamoir, F.(1)*;De Leuze, F.(1);Denis, M.(1);De Vroey, B.(1);De Suray, N.(1);Burnet, G.(1);Piessevaux, H.(1);Dewit, O.(1);
(1)Cliniques Universitaires Saint-Luc, Gastro-enterology, Brussels, Belgium;
Background
Anti-tumor necrosis factor (TNF)-α agents are a therapy of choice in the induction and maintenance treatment of inflammatory bowel disease (IBD). Unfortunately, their efficacy varies. Some IBD patients are primary non-responders and many will experience a secondary loss of response. However, we do not yet have good predictors of their efficacy. Obesity, which prevalence increases worldwide, is also increasingly found in IBD population. Some studies suggest an association between obesity and poorer response to anti-TNFα therapy in IBD patients, although with conflicting results.
The aim of this study is to assess the impact of patients’ body mass index (BMI) on the efficacy of anti-TNFα agents in IBD and if there is difference according to the route of administration (intravenous (IV) vs subcutaneous (SC)) or the type of disease (Crohn’s disease (CD) vs ulcerative colitis (UC)).
Methods
We retrospectively collected data from 188 patients with IBD, aged ≥ 18 years, treated with a first anti-TNFα agent started in our center between January 2002 and December 2020 to avoid missing data. A lack or loss of response to anti-TNFα therapy was defined by the need to optimize or change the treatment or by the initiation of any intercurrent treatment (steroid therapy, hospitalization, or surgery). Frequency of the event and time to its occurrence were analyzed and compared according to BMI using uni- and multivariate logistic regression models and survival curves (Kaplan-Meier), represented by BMI categories (<18.5; 18.5-25; 25-30 and ≥ 30 kg/m²).
Results
In this cohort of 188 patients (143 CD, 43 UC, 2 Indeterminate Colitis), 8% were obese. We observed that the higher the patient's BMI, the earlier the risk of optimization or change of treatment (HR=1.043, p=0.045). Association was even stronger for obese patients (HR=2.13, p=0.018). After adjustment for IBD type and administration route, association with obesity persisted.
Two other characteristics - female gender (HR=1.56, p=0.012) and higher CRP (HR=1.14, p=0.021) – were associated with earlier optimization or treatment change. Similarly, analysis of survival curves showed a significant difference in time to optimization or change of treatment between BMI categories in patients with CD (p=0.02) but not in those with UC (p=0.87). 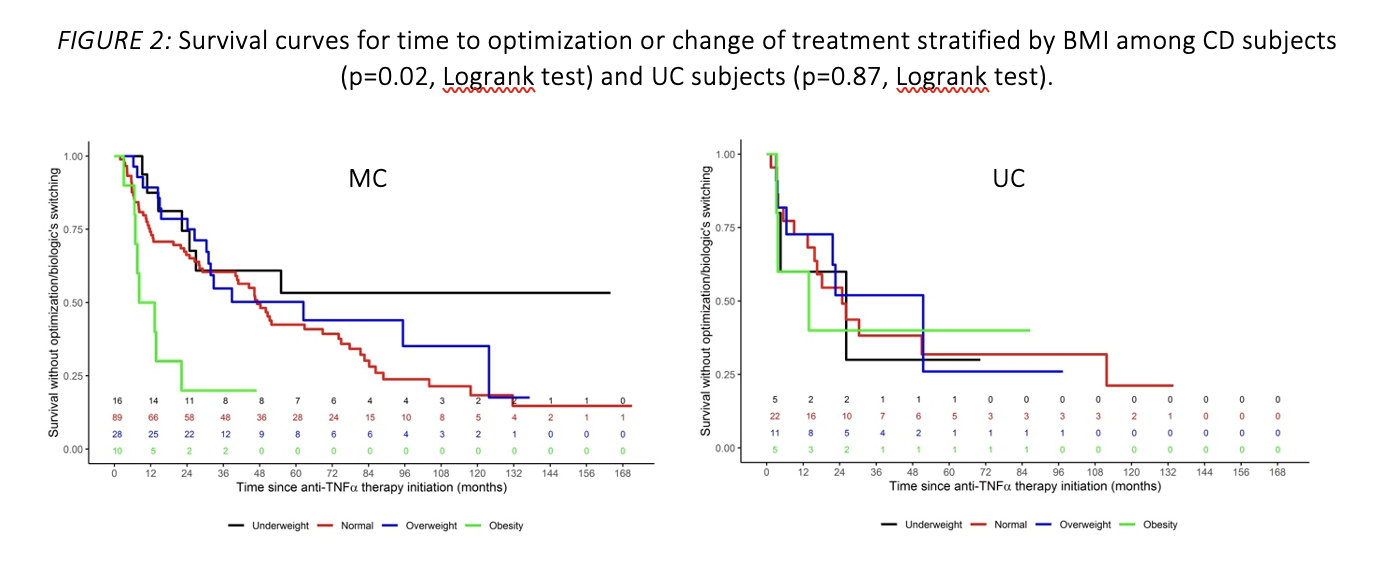
No association was found between BMI and need for intercurrent treatment.
Conclusion
This study confirms an association between higher BMI – specifically obesity - and an earlier loss of efficacy of a first anti-TNFα treatment, regardless of IBD type or route of drug administration. Prospective studies with analysis of trough levels are required for a better understanding of the mechanisms involved in the response to anti-TNFα therapy in IBD obese patient.


