P622 Change in Dietary Inflammatory Index Score in patients with Crohn’s disease and healthy volunteers following the Groningen Anti Inflammatory Diet (GrAID)
BarthDrs., I.(1)*;Stevens, C.L.(1);Campmans-Kuijpers, M.J.E.(1);Dijkstra, G.(1);
(1)University Medical Center Groningen, Gastroenterology and Hepatology, Groningen, The Netherlands;
Background
Dietary patterns play an important role in Inflammatory Bowel Disease (IBD). The Dietary Inflammatory Index (DII) is a diet quality score that estimates the inflammatory potential of a dietary pattern on inflammatory markers. Recently, the Groningen Anti-Inflammatory Diet (GrAID) was developed to improve disease course in patients with IBD. The aim of this study is to investigate whether following the GrAID improves diet quality based on the DII compared to baseline intake in patients with Crohn’s disease (CD) and healthy volunteers (HV).
Methods
Between October 2021 and October 2022, patients with CD and HV completed a 12-week GrAID intervention as part of an ongoing trial: VITA-GrAID (NCT04913467). In this sub analysis, nutrient intake from a 3-day food diary was calculated at baseline (T0; habitual diet) and after 12 weeks (T3; following the GrAID), using Evry software (version 2.3.7.0). From both intakes the DII score according to the Shivappa method was calculated, based on 28 food parameters. Next, both scores were compared to the DII score of the GrAID, calculated assuming complete adherence to the GrAID. A lower DII score is regarded to having a higher anti-inflammatory potential. Paired nonparametric tests (Wilcoxon signed-rank) were performed to calculate differences between T0 and T3. Data were analysed using R (2021.09.0) and IBM SPSS Statistics 28.
Results
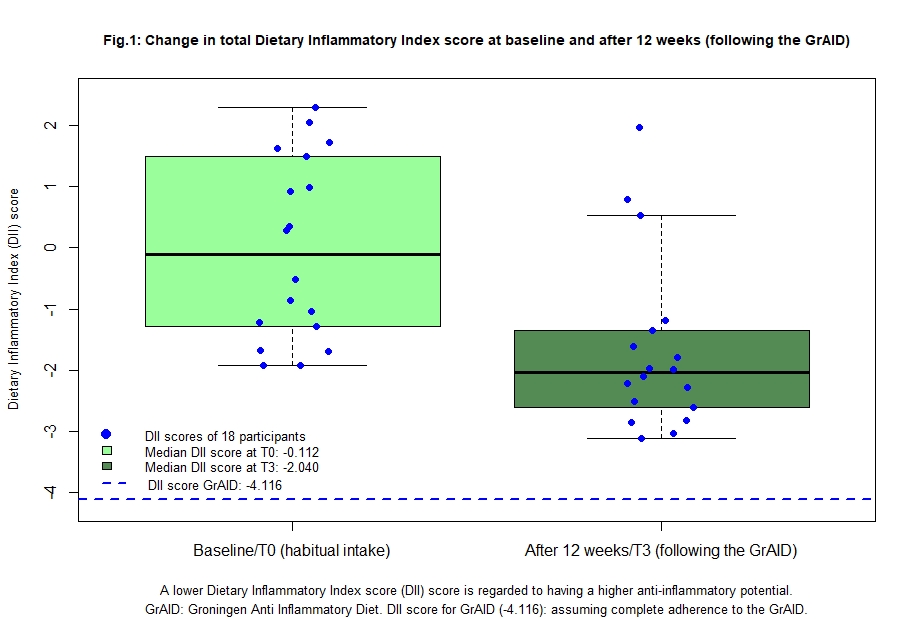
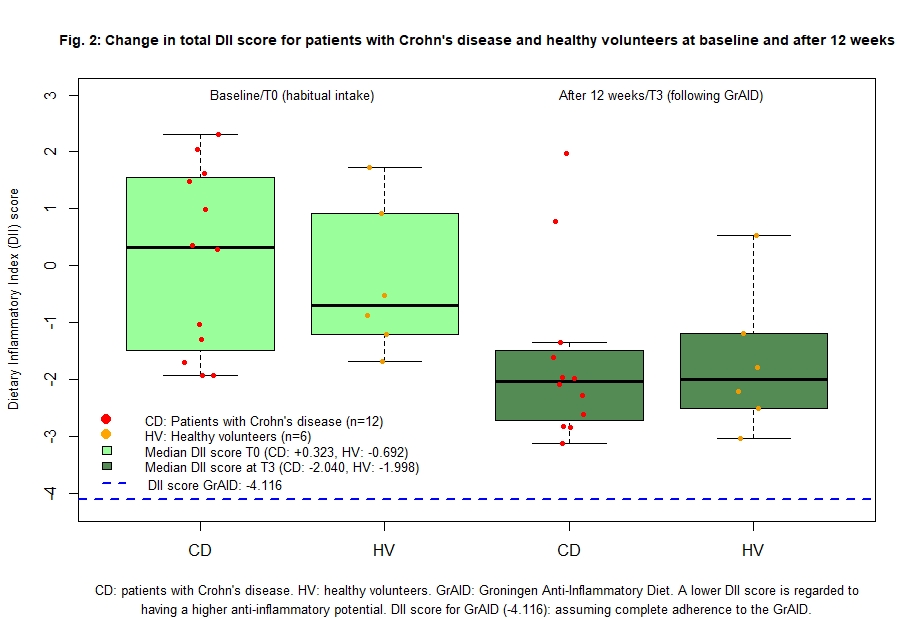
Eighteen individuals completed the 12-week GrAID intervention (12 patients with CD; and 6 HV) (table 1). Between T0 and T3, significant increases were found in fibre (16.5g), total protein (21g), total plant protein (14g), vitamin B2 (0.29ug) and beta carotene (1837ug) intake. Significant decreases were found in mono- and disaccharides (-18g), alcohol (- 5.3g), and sodium (-875mg) intake (Table 2). The median DII score at T0 was -0.112, IQR: [-1.269; 1.362] and was significantly lower at T3 (median: -2.040; IQR [-2.588; -1.417], p<0.05) (figure 1). Median DII score in patients with CD differed significant between T0 and T3 (0.323, IQR [-1.3897; 1.523] and -2.040, IQR [-2.665; -1.549] respectively, p<0.05), but not in HV (-0.692, IQR [-1.127; 0.566] and -1.998, IQR [-2.441; -1.336] respectively, p=0.09) (Figure 2).

Conclusion
These preliminary results show that diet quality improved in patients with CD after following the GrAID for 12 weeks. For HV, probably more participants are needed. Further research is necessary to determine whether a lower DII score will actually improve the disease course of patients with CD and the diversity of the microbiome in HV.


